Theme Leader :
Hirohiko Hirano, D.D.S., Ph.D.
Vice-Chief Researcher:
Keiko Motokawa, R.D.N., Ph.D.
Researcher :
Maki Shirobe, R.D.H., Ph.D.
Adjunct Researcher :
Ikuo Nasu, D.D.S., PhD., Masanori Iwasaki, D.D.S., PhD., Kentaro Igarashi, D.D.S., PhD., Shiho Morishita, R.D.H., PhD., Chiaki Matsubara, R.D.H., PhD., Eri Sanbuichi, R.D.H., PhD.
Other Research Staff:
Yurie Mikami, R.D.N.
Oral Frailty, Healthy life expectancy, Dementia, Home care, End-of-life care, Appetite, Behavioral and Psychological Symptoms of Dementia for eating, Malnutrition, Dietary variety, Dysphagia diet, Oral function, Oral related health literacy, Community care, Day care
1. Research on improvement of oral function and nutrition in the older adults
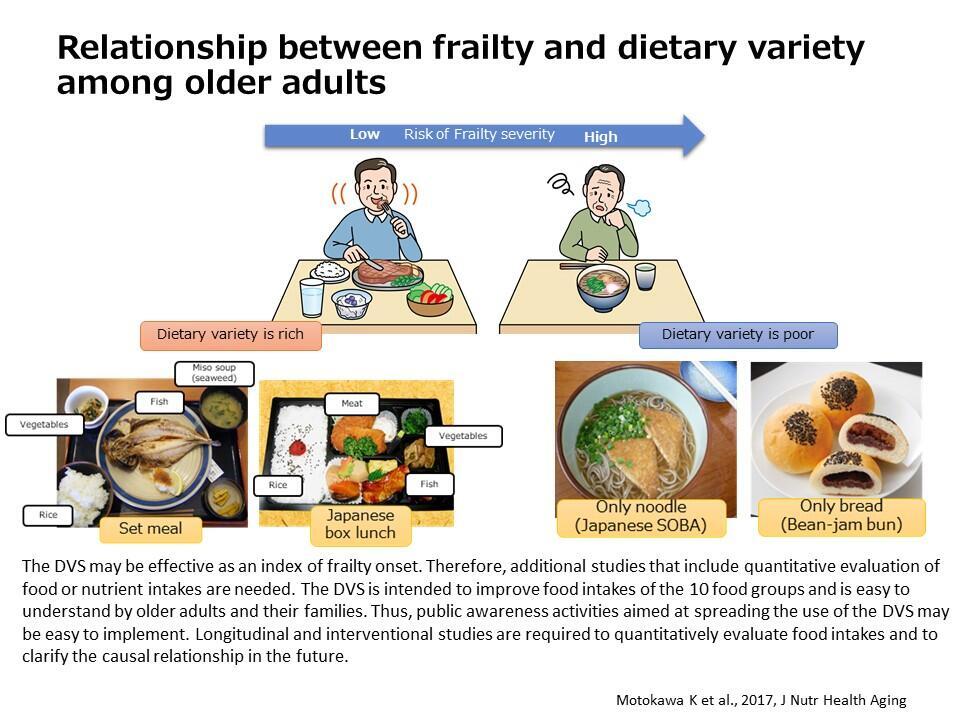
This research aims to establish methods forevaluating oral function and nutritional status, to develop and validate oral frailty prevention programs, and to design regulated diets that consider food texture and swallowing function. Oral frailty, a concept originally proposed in Japan, refers to a state of oral function between the normal condition of a "healthy mouth" and the "decline of oral function." We are developing and validating an index to assess oral function and nutrition among healthy older adults, frail older adults, and those requiring long-term care, with the goal of promoting its widespread use across community, long-term care, and clinical care settings.
Regarding oral frailty and related prevention programs, we are conducting a large-scale collaborative project with multiple research institutes. Our objective is to promote broad understanding of oral frailty and to facilitate implementation of prevention programs not only in Japan but also across other Asian countries.
Our research on regulated diets that incorporate food texture and swallowing function identifies key issues based on large scale fact-finding surveys and conducts multifaceted analyses on strategies to address these issues in community settings, with the ultimate aim of supporting practical implementation.
2. Research on oral and nutritional support for older adults with dementia
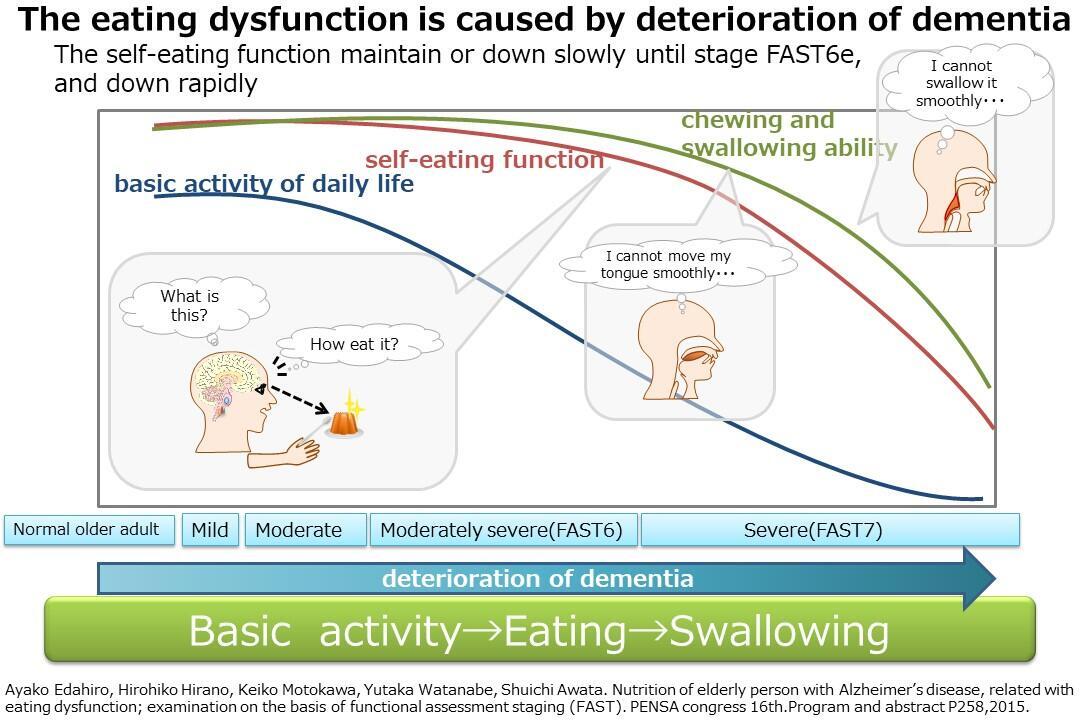
This research aims to clarify various issues related to oral intake in older adults with dementia, including those arising from neuromuscular symptoms and drug side effects, and to obtain collective intelligence regarding evaluation and intervention measures through multidisciplinary collaboration.
To address the identified issues, we have developed guidelines on dental treatment and other oral care for older adults with dementia. Using data collected from nursing-care insurance facilities, group homes, and similar settings, we are analyzing information on dementia diagnosis, stage, and clinical status, as well as medication, symptoms of oral intake difficulties, and interventions.
Through multidisciplinary collaboration involving families and caregivers, we aim to establish comprehensive support methods that integrate both oral health care and nutritional management, including assessment and intervention strategies, so that older adults with dementia can continue to live safely intheir familiar communities.
3. Research on oral health and nutrition policies
This research aims to evaluate the effects of policies related to oral health and nutrition, including medical and nursing care fees, identify new issues and other institutional problems related to oral health and nutrition, and establish a foundation for revising medicaland nursing care fees.
In addition, with the goal of further promoting an integrated community care system, we are conducting research to assess oral intake and nutritional status, support continued homecare, and increase the availability of nursing care, targeting older adults from healthy individuals to those requiring long-term care.
Specifically, we aim to contribute to the development of human resources and regional services, clarify the role of nursing care facilities, promote an integrated community care system, and maintain medical and long term care insurance services, thereby ensuring that older adults receive the oral and nutritional care necessary to continue living as they wish.